
First they come for the proceduralists
March 12, 2021
Vaccine hesitancy in the age of COVID-19
March 12, 2021FEATURE
General practitioner and former AMA (NSW) President, Dr Brian Morton shares his step-by-step preparations to run COVID-19 vaccinations at his Sydney practice.
All of us have been waiting for the availability of a vaccine for relief from the COVID-19 pandemic. We have been told it’s the long-term solution to opening the borders and life returning to a semblance of normal. And just a little over a year since COVID hit our shores, it appears we’re on the cusp of being able to immunise patients from the worst of this disease.
Australia has secured 53.8 million doses of the AstraZeneca vaccine, of which 50 million doses are to be made locally. The Commonwealth recently confirmed that the CSL facility in Melbourne was on track to deliver the first batch of doses to a limited number of general practices in the week starting on 22 March.
There seems a moral imperative as a medium size general practice to provide a vaccination clinic available to not just our practice patients but also the local community. Our practice, which is located north of Sydney, has 10 general practitioners who have amalgamated from separate practices in adjacent communities. All of the original practices have been in the area for 40 years and we have been in our current location since 2008. Given this history, we are well-established in the community and have a strong patient base.
It became obvious from the EOI process that running COVID-19 vaccinations at your practice was not going to be ‘business as usual’. Hence, a considerable amount of planning has gone in to preparing our practice to accommodate the vaccine rollout.
In order to successfully incorporate COVID-19 vaccinations into our practice, we developed a strategy that would allow us to not only provide this service to our patients, but also allow us to carry on with our regular appointments.
Here is a step-by-step breakdown of our preparations to date:
Step 1: Finding space
Fortunately, our building has vacant office space, so our practice manager asked the landlord for access and we were generously given permission at no rental cost.
Step 2: Developing a plan
We held a practice meeting to reach agreement with all our staff and GPs to action a clinic. All agreed with both the principle and the functional plan. It was agreed that separation of the COVID vaccination clinic from normal daily activity would be essential.
Step 3: Ordering supplies
At the time of writing, we had just received confirmation from the Federal Government as to when we would receive our vaccines and how many doses we would be able to provide to patients. But in the weeks leading up to this, we set about ordering the supplies we would need to maintain a surgically clean environment.
Step 4: Storage capacity
We next turned our thoughts to freeing up space in our two vaccine refrigerators. We have some additional availability given that travel vaccines have not been needed, and we have been allowing routine vaccine quantities to be reduced.
Step 5: Bookings
We are also anticipating increased calls from patients who are looking for more information about COVID vaccinations and bookings. To deal with this, we put in place a telephone message, which instructs callers to go to our website for information about the clinic and for online bookings.
Step 6: Updating our website
In order to provide patients with the most up-to-date information as possible, we are putting together some unique content on our website, which will provide background information on the vaccines, the COVID-19 Vaccine Rollout strategy and patient prioritisation and booking information.
Step 7: Assessing the layout of the clinic space
This includes looking at patient flow through the clinic from the registration desk, pre-vaccine waiting area, two vaccination rooms set for privacy, post-vaccination waiting area, and then the exit desk.
Step 8: IT connectivity
We identified that we will need two laptops. One to be used for patient identification, eligibility and registration, and the other for inputting to the Australian Immunisation Register and the doctor’s clinical notes.
Step 9: Staffing
To run the clinic as efficiently as possible, we determined we will require a receptionist (R), practice Nurse (N), GP 1 (D1) and GP 2 (D2).
Step 10: Rostering
Based on the staffing requirements outlined above, we developed this schedule: See chart below.
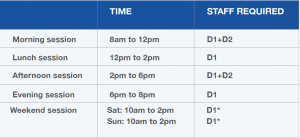
*Schedule is subject to change according to staffing availability and demand
Step 11: Bookings
Once we have received the vaccines and are ready to go, then we will need to go through our patient base and identify those who are eligible patients in Phase 1b of the COVID-19 Vaccine Rollout Strategy and create a listing for calls for attendance.
We are anticipating we will need approximately five minutes per patient for the vaccination and our bookings will be made to reflect that.
What’s next?
There will be other considerations and processes that will need to be put in place, but this is a brief skeleton of our practice’s logistical strategy thus far. Of course, further considerations will have to be made and we anticipate there will be some learnings along the way.

